Antibiotic Resistance Breakers

WRITTEN BY:


An Orthogonal Approach To Antibiotic Discovery
ARBs, sometimes referred to as antibiotic adjuvants, are non-antibiotic moieties which do not have any antimicrobial activity on its own, but, in combination with antibiotics enhance their antimicrobial activity and help overcome resistance barriers.
Types of ARBs
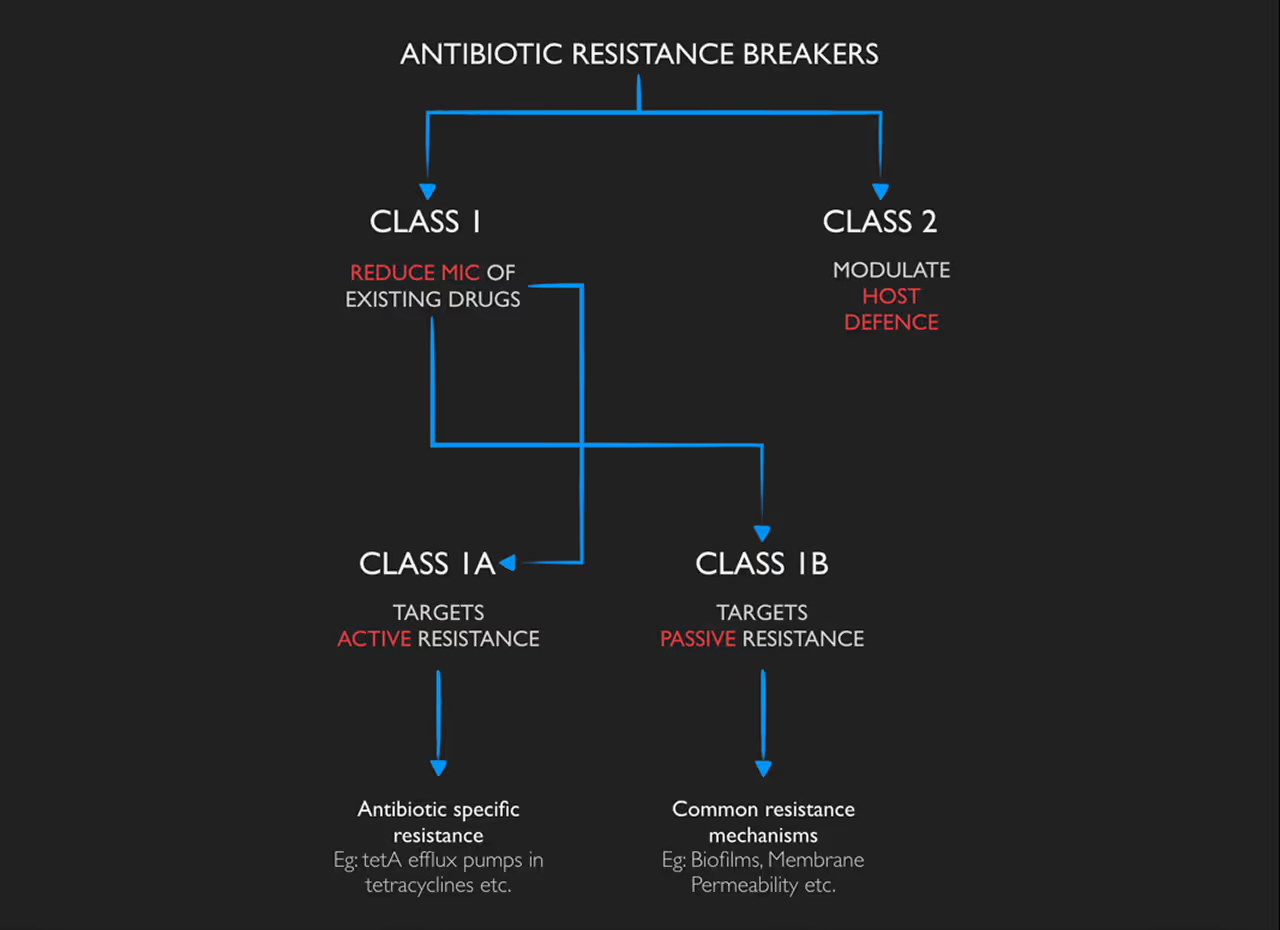
They can broadly be classified into 2 classes - Class 1 ARBs that help reduce the MIC of existing antibiotics (when used in combination), and Class 2 ARBs that act on hosts' defense mechanisms.
Although the term Antibiotic Resistance Breakers is relatively new, the concept itself dates back to the early 1970s when the first beta-lactamase inhibitors (BLIs) were developed.
Most BLIs can be thought of as ARBs that do not have any significant antimicrobial activity when used alone, but in combination with a beta-lactam antibiotic, help restore the activity against beta-lactamase producing organisms.
ARBs should be sought to salvage one or more key members of each mechanistic antibiotic class, particularly those used against Gram-negative bacteria. Thus, the antibiotics that most need ARBs are: cephalosporins and carbapenems (which disrupt cell wall synthesis); polymyxins (which disrupt cell membrane synthesis); fluoroquinolones (which disrupt DNA synthesis); tetracyclines and aminoglycosides (which disrupt protein synthesis by inhibiting the 30S ribosomal subunit); and macrolides (which disrupt protein synthesis by inhibiting the 50S ribosomal subunit).
ARBs that help in restoring activity against K. pneumoniae, E. coli, P. aeruginosa and A. baumannii, the four Gram-negative organisms whose resistance to antibiotics is of greatest concern (all of which produce carbapenemases and are thus resistant to many β-lactam antibiotics), are of utmost importance.
Traditional Vs ARB Approach
Repurposing drugs using ARBs overcomes many of the commercial barriers to developing new antibiotics and it is estimated that the use of ARBs could salvage many of the 200 or so existing antibiotics for the future generations.

Reasons to support the development of Antibiotic Resistance Breakers:
- Resistance to current antibiotics is rapidly increasing. Discovering new classes of antibiotics with novel mechanisms of action poses tremendous challenges as the scientific, commercial, and regulatory conditions are not presently aligned for the discovery of new drug classes
- ARBs can be combined with existing antibacterial agents with known pharmacological and toxicological effects, leading to considerable cost savings by eliminating much of the toxicological and pharmacokinetic assessments that would normally be required for the approval of a new drug or combination, thereby reducing the time to market
- ARBs would be particularly useful as their development could be faster, cheaper and provide a higher probability of success than that for new molecules
- If resistance develops to the first ARB combination, a second ARB could potentially rescue the same antibiotic. This cycle could be repeated many times, enabling old antibiotics to be used far into the future.